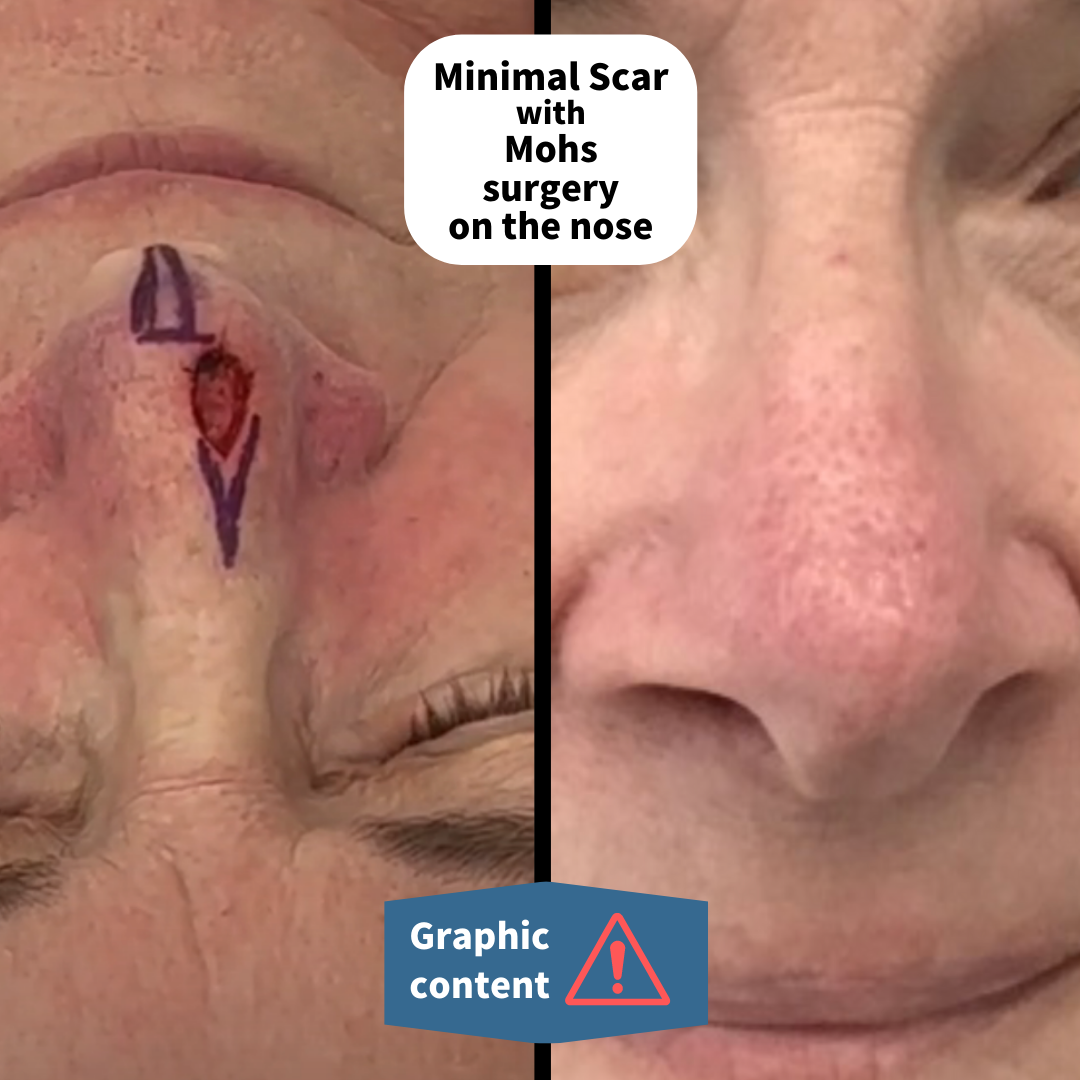
Pam came in with a spot on her nose. She didn’t think it was a serious problem at first.
“You know occasionally you have a pimple or something. This was something like that, and I will usually use a little neosporin or lavender oil, and it usually clears up. But this thing… didn’t respond at all. It was this little pit with black down in it and it didn’t scab. After about a month, I saw my family practice doctor who sent me here (to Ada West Dermatology,)” Pam explains.
Family History
Pam was aware of skin cancer in her family. She says, “My mother had a lot of skin cancer. And I was the person who brought her in and sat with her. She was very dark skinned and also spent a lot of time in the sun working in the local orchards as a kid.” Pam explains she remembers her mother’s skin cancer on her nose. That one needed 5 separate cuts and a skin graft.
Her hopes were that the surgery would be less of an ordeal than what she saw her mother go through. Thankfully, Mohs micrographic surgery has been refined since then into the most precise and advanced treatment for skin cancer with success rates up to 99 percent while preserving all the healthy tissue possible. Pam was also nervous about any pain she might feel, but gratefully, most patients feel very little as their treatment area is well-numbed before the surgery. “Dr. Thorpe does a fantastic job in making the surgery as comfortable as possible. As I watched the video I thought, ‘Wow– it didn’t hurt!’”
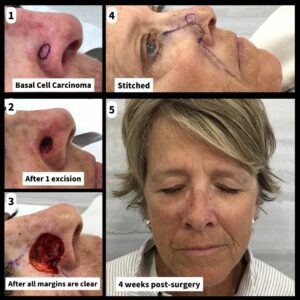
Pam’s original biopsy showed basal cell carcinoma (BCC). Unlike melanoma, BCCs rarely spread beyond the original tumor site. But these lesions can grow and become disfiguring and dangerous. Untreated BCCs can become locally invasive by growing wide and deep, destroying skin, tissue (nerves/muscle/fat/cartilage/etc) and even bone in the process.
Mohs Process
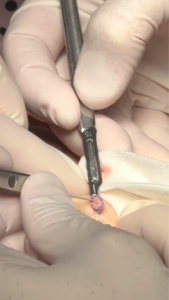
Dr. Thorpe begins by removing a thin layer of the visible cancer and sending it to the in-house Mohs lab. In the lab, our technician freezes the divided tissue, then cuts very thin slices, with each slice representing the pie crust of the pie. In this way, Dr. Thorpe can evaluate 100% of the margin. The slices are placed on microscope slides, stained and then given a coverslip. This meticulous process allows Dr. Thorpe to examine all the edges and see if any cancer cells remain. If there is more cancer, another layer is taken – but only where the cancer remains – and the process repeats itself until the patient is completely cured of the cancer.
In Pam’s case, two layers were required to clear the cancer.
Once the site is clear of cancer, the wound is closed with stitches (depending on size and location). In Pam’s case, you’ll see that Dr. Thorpe used a type of repair called a Burow’s advancement flap. He chose this flap to maintain the contours and symmetry of the nose from all directions. Care is taken to make the correct plan before proceeding. Once the plan is decided, the flap is incised, the area is undermined, bleeding is controlled, and then multiple layers are placed to achieve the best cosmetic outcome possible.
About Basal Cell Carcinoma
Basal cell cancer is the most common form of skin cancer, accounting for nearly 80% of all skin cancers. Basal cell cancer gets its name from the cells it comes from, which is the bottom layer or basal layer of the epidermis. While it is rarely fatal, it can be locally aggressive.